I’ve come across a concerning trend in my practice lately…. that is, patients assuming that all low-back pain is the same, and therefore all low-back pain solutions are the same.
Low back pain (LBP) is most definitely the number one condition that walks into my office, even though we offer a full-body approach; from necks to toes and everything in between. But here’s my concern: please don’t assume that your low back pain is the same as your friend’s low back pain. Just as you wouldn’t take a friend’s prescribed medication, be wary of taking a friend’s prescribed rehabilitation exercises. I hear this all the time: “My friend told me to do ____ for their back pain.” “I saw this stretch on Google.” “My sister had back pain and she still did 100 sit-ups a day.”
Please, no. (And also, please, please, please, NO sit-ups. Ever. We can talk about this later. Email me.)
Don’t assume that your back pain is the “same” as your friend’s/neighbour’s/Uncle’s/dog’s. There are many causes of low back pain, and it’s my job to figure out what is causing yours specifically, and give you the appropriate rehab to support that. In certain cases, forward fold stretches can be helpful. In certain cases, they can be harmful. The same can be said for extension exercises, and mobility drills, and activity limitations. Each has their time and their place, and one size does not fit all.
Low back pain is a widespread condition; in fact, up to 85% of working Canadians can expect to experience LBP in their lifetime. And if we all work together, from practitioners to researchers to personal trainers to patients, I think we can dramatically lower that statistic.
There is one hard and fast rule that everyone can safely adhere to: a neutral spine is always the most preferred, protective posture for your spine. Keep that in mind the next time you sit, stand, bend, lift, or twist.
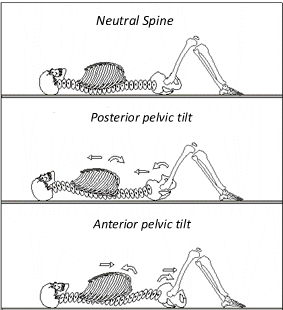
Happy Tuesday.




 You see, our bodies are very, very smart. They know what to do to fix things, far better than I claim to know. But the thing is, our bodies don’t take compensation injuries into account. A rob-Peter-to-pay-Paul situation often develops. And let’s not forget the time factor; manual therapy can speed up healing rates.
You see, our bodies are very, very smart. They know what to do to fix things, far better than I claim to know. But the thing is, our bodies don’t take compensation injuries into account. A rob-Peter-to-pay-Paul situation often develops. And let’s not forget the time factor; manual therapy can speed up healing rates.